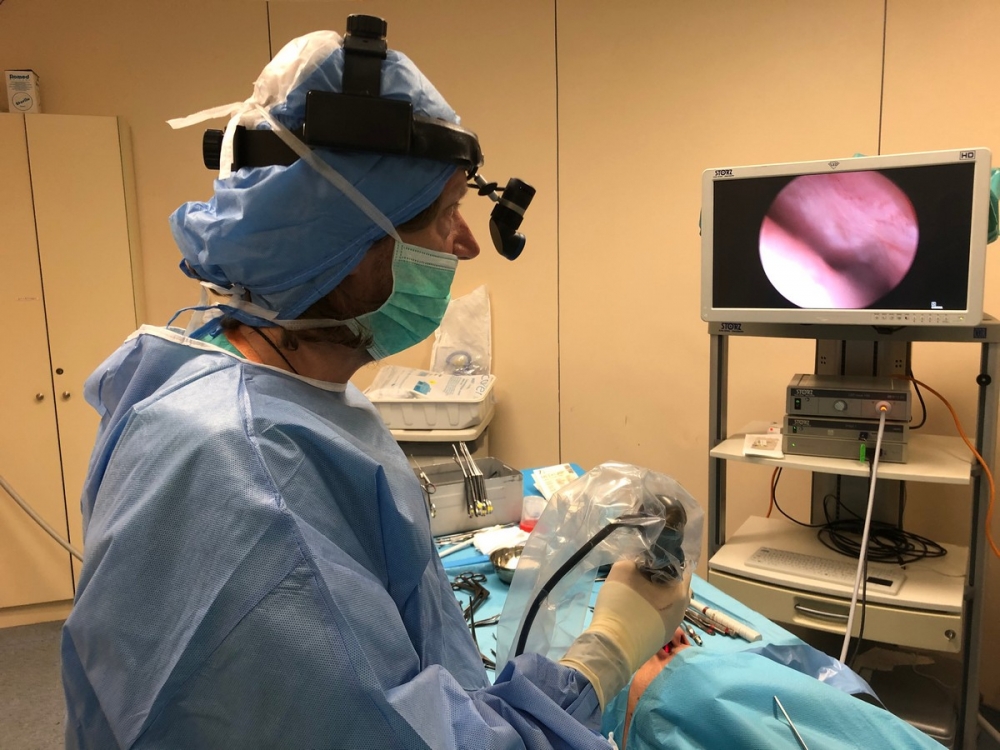
Snoring and apnea consulting room
Home » Snoring and apnea consulting room
You should first arrange an appointment with the doctor and discuss your problem with him. The doctor will be able to inform you on the causes and parameters of your snoring and/or apnea problem.
Then, you can look on the high-definition video camera and see which anatomical part (uvula, tonsils, diaphragm, conchae, adenoids) is responsible for your snoring or/and apnea problem. Thanks to its very small diameter (only 3.2 mm), the latest Olympus flexible video camera ensures an easy, painless and quick scanning of the entire upper airway, from the nose entrance to the larynx glottis and the trachea entrance, without disrupting any of the anatomical elements, since the scanning is done in one and only single passage.
Also, thanks to the special hydrophilic shell and the soft texture, the flexible camcorder slides more easily through the soft airway particles, thus making the examination completely painless. The only thing that is required for the examination is a mild local anesthetic in the nose with a cotton pledget impregnated with xylocaine.
Depending on the findings of the test, the physician can then inform the patient on how possible it is to treat the causes of his/her snoring or apnea with the most modern surgical methods. Flexible endoscope scanning can be combined with the seated or supine Müller test which gives more information on the level of the upper airway obstruction; especially in severe obstructive apnoeic syndromes, there are more than one levels of obstruction. The endoscopic video is sent to you in digital format (email) by the office’s secretary.
In case of suspected airway obstruction low in the larynx, in the epiglottis or by contraction of the lateral hypopharyngeal walls or when a treatment has already failed, suspicions then can turn into indications with the drug induced sleep endoscopy (D.I.S.E). Thanks to the “sleeping simulation” it generates, this special type of diagnosis accurately reveals the levels of airway obstruction that can cause obstructive sleep apnea, especially when this is located deep into the larynx.
In case of suspicion of sleep apnea episodes, then patients can immediately get the Snore-Check devise from the consulting room and submit themselves to sleep sonography - digital sleep recording and sleep analysis. The results are then analysed by the Medical Center for Sleep and Primary Care and are communicated to the patient the next day. The Snore-Check sonography serves as a screening test, in order to confirm the need for conducting a regular Sleep Study in the case of a serious apnea syndrome.
In severe cases of snoring and in cases of obstructive sleep apnea (OSA), the use of surgical ultrasound has been the ideal choice for application the last few years. It is a state-of-the-art device consisting of a generator that generates high-frequency oscillations that are transmitted to the ultrasound cutting instrument, which in turns interferes with the anatomical barrier that is responsible for snoring (uvula, tonsils, nasal conchae, nasal bone spur etc). Usually, a simple uvula excision needs to be performed in order to stop snoring permanently. Occasionally, a soft plastic surgery in the palate arches or shrinkage of the tonsils may be needed in order to open more the airway. The whole procedure is completely bloodless, painless and does not last more than 15-20 minutes. In some cases, the procedure can be done without the use of general anesthesia – just combining a local and regional anesthetic. A few hours after the procedure is done, the patient can go home. The results are immediate and the patient is relieved of snoring from the very first night. Postoperative pain, which is much softer than in the classic surgery, lasts only for a few days, during which the patient must follow a special diet with slurry and warm foods.
Are you looking for answers and seeking a solution to your health concerns?
Monday to Thursday: 5 pm - 8 pm and Friday: 10:30 am - 1 pm
Call usOR
Please fill out the contact form: